Frank Gaglioti
The SARS-CoV-2 virus that causes the disease COVID-19 is nimbly and stealthily racing through community after community devastating the world’s population. Over 23 million people have contracted the virus worldwide and 810,000 have died. It is critical to review the evolutionary history of this particular virus to provide necessary insights into how the pandemic can be brought under control.
Researchers worldwide are working arduously to trace the virus globally by studying samples obtained from various nations looking for subtle mutations that it undergoes as it infects, replicates and multiplies, providing them clues to the source and route of spread.
COVID-19 is caused by a type of coronavirus known as SARS-CoV-2, named for its similarity to the coronavirus that caused SARS. The virus is called a coronavirus because it is covered by club-like structures that give the virus a similar look to the sun’s corona in electron micrographs.
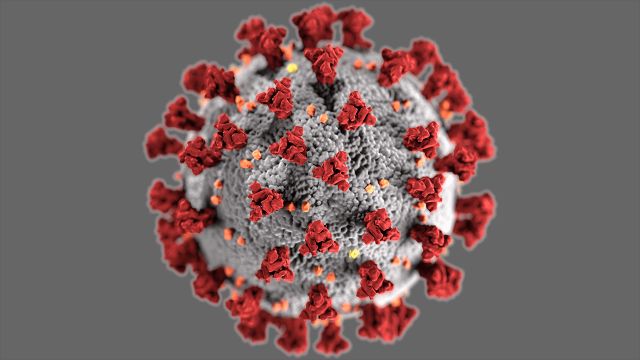
The SARS-CoV-2 virus is part of a family of organisms that are known to infect mammals and birds. The Coronaviridae family are made up of a positive-sense single-stranded RNA completely enveloped in a complex protein and bilipid shell. These viruses are relatively large, consisting of 26 to 32 kilobase pairs. RNA or ribonucleic acid is a nucleic acid that is essential for all reproductive processes and like DNA.
The first known scientific encounter with this family of virus is thought to be when veterinarians puzzled over bronchial infections afflicting cats, pigs, and chickens in the early 20th century.
Study of disease afflicting and damaging tobacco crops in the late 19th century led some thoughtful scientists like Dimitri Ivanovsky to conjecture the existence of non-bacterial infectious agents causing the “tobacco mosaic disease.” It would take another 50 years to capture the first images of the Tobacco Mosaic Virus. The invention of the electron microscope in 1931 enabled scientists to observe viruses more closely, allowing a more extensive and direct study of these micro-organisms. Virology as a field began to flourish.
Human coronaviruses were first identified in the 1960s. Seven species of coronavirus are known to afflict humans. Four result in relatively mild upper respiratory tract conditions, including the virus 229E that causes the common cold, along with NL63, OC43 and HKU1.
The other three strains, SARS, MERS, and SARS-CoV-2, are far more virulent. All these viruses were new to human populations when they first arose in the 21st century. A feature of SARS, MERS and COVID-19 is that they had a zoonotic origin, that is they originated in animal populations and then jumped into humans. The SARS outbreak in 2002, with a case fatality rate of 11 percent, showed the world the deadly potential of coronaviruses, but this was a warning that was mostly ignored. There had only been 8,422 cases and since 2004 no SARS-CoV has been reported worldwide. One advantage for public health responses to SARS was that it had an incubation period of 4 to 6 days and patients presented with symptoms prior to becoming infectious.
In their extensive investigations, the World Health Organisation (WHO) concluded that the SARS virus originated in bat populations, but the exact species remains unknown. Work commenced on the development of a SARS vaccine with testing on animals. The vaccine resulted in protective immunity but produced an immune mediated hypersensitivity as an adverse effect. The SARS threat, for unknown reasons, expired after six months though limited outbreaks did occur later.
With the threat of a pandemic having ended after six months, so did any interest in funding a vaccine, as pharmaceutical companies saw no profit in funding or exploring such research. The co-director of the Center for Vaccine Development at Texas Children’s Hospital and dean of the National School of Tropical Medicine at the Baylor College of Medicine in Houston, Dr. Peter Hotez, had been attempting to develop a SARS vaccine in 2016 but couldn’t get funding for his work. “We tried like heck to see if we could get investors or grants to move this into the clinic ... But we just could not generate much interest,” he said.
“We could have had this ready to go and been testing the vaccine’s efficacy at the start of this new outbreak in China (COVID-19) … There is a problem with the ecosystem in vaccine development, and we’ve got to fix this,” Hotez said.
The genomic sequence of the SARS virus was published in August 2003 by Chinese scientists in Beijing. In actuality, when the cause of the pneumonia-like illness was first identified in Wuhan, some believed this was a new outbreak of the SARS virus. SARS-CoV-2 and SARS share a genomic sequence that is approximately an 80 percent match.
Middle East Respiratory Syndrome, or MERS, emerged in Saudi Arabia in 2012 and had a zoonotic origin in bats and was spread to humans through contact with dromedary camels. The virus produced symptoms similar to SARS but it had a low infectivity though highly lethal. Of the reported 2,500 cases, 35 percent died from the disease.
With limited capacity to spread from human to human, it was mainly passed through contact with infected people in hospitals. In the main it was concentrated in the Arabian Peninsula, although there were further outbreaks in South Korea in 2015 and Saudi Arabia in 2018. It continues to smoulder in the Middle East.
When the SARS CoV-2 virus emerged in late 2019, the world was totally unprepared. Health systems internationally had been systematically run down and were ill-equipped to respond. The warnings from WHO of the dangerous potential of the virus were largely ignored or belittled. The murderous government policies that dominated have been described as malign neglect or herd immunity.
SARS CoV-2 arose in Wuhan in December 2019. The virus is thought to have originated from bats and to have transferred to humans through an intermediary species. The exact origins of the virus may never be known. “It is quite possible we won’t find it (the species). In fact, it would be exceptionally lucky if we land on something,” a geneticist from University College London, Lucy van Dorp, told Nature .
Back in 2013, the Wuhan Institute of Virology had investigated the coronavirus genome from the horseshoe bat ( Rhinolophus affinis ). The viruses named RATG13 and SARS-CoV-2 were found to be 96 percent genetically similar. There are, however, subtle molecular changes that continue to be investigated that contribute to selection pressures that drive the virulence, pathogenicity, and immunogenic qualities of the virus.
In their detailed analysis of the origin of the SARS-CoV-2 virus, Andersen et al., 2020, offered three possible explanations: 1) natural selection in an animal host before jumping into humans, 2) natural selection in humans after the virus transferred into human hosts, and 3) the product of artificial manipulation, which has been refuted by several virologists. According to Van Dorp, “… the 4% difference between the genomes of SARS-CoV-2 and RATG13 still represents some 50 years since they last shared a common ancestor.”
It was thought that pangolins ( Manis javanica ), a scaly ant-eating mammal, may be the intermediate host between bats and humans, but genetic studies indicate that as unlikely. However, some scientists think that because coronavirus-like SARS-CoV-2 cases have been found in pangolins, that species cannot be ruled out as the intermediary source.
Scientists are currently examining species of animals that were kept and sold in the live markets in Wuhan where bats may have been in the buildings’ roof near animals and humans. Presently a team of experts from the WHO are working with their Chinese counterparts to answer this pressing question.
“The opportunities for these viruses to spill over across a very active wildlife-livestock-human interface is clear and obvious,” the president of the EcoHealth Alliance in New York City, Peter Daszak, told Nature. The complex evolutionary history of SARS-CoV-2 disproves President Donald Trump’s ignorant claims (which have a political purpose) that the virus came out of a Chinese laboratory. “Whether they [China] made a mistake, or whether it started off as a mistake and then they made another one, or did somebody do something on purpose?” Trump said.
In a recent paper published in Nature Microbiology —“Evolutionary origins of the SARS-CoV-2 sarbecovirus lineage responsible for the covid-19 pandemic,” led by Maciej F Boni from the Center for Infectious Disease Dynamics at Pennsylvania State University—found that the lineage of SARS-CoV-2 had been circulating in bat populations for decades. “If these viruses have been around for decades that means that they’ve had lots of opportunity to find new host species, including humans,” said Professor David Robertson from the University of Glasgow.
Scientists have carefully examined the Receptor Binding Domain (RBD) of the genetic sequence that codes for the spike protein, the necessary structure on the virus’ exterior shell that is used to bind and penetrate the human cell. The spike protein has been compared to a grappling hook that grips the host cell, then creates a cleavage site that enables the opening and penetration into the host cell.
This means that the SARS-CoV-2 spike proteins had evolved to target a feature of human cells known as angiotensin converting enzyme 2 receptor (ACE2) which are well known to assist in regulating blood pressure.
Andersen et al ., remark that the RBD is the critical component of the spike protein that allows it to bind to ACE2 receptors. SARS-CoV-2 appears to bind with great affinity to the human ACE2 receptors, but computational analysis predicted that the interaction is not ideal. According to the New York Times, “the authors indicate that the high-affinity bindings of the virus’ spike protein to human ACE2 is most likely a by-product of natural selection that has permitted another ‘optimal binding solution to arise.’ They then conclude that this is strong evidence that SARS-CoV-2 is not a product of genetic reconstruction or tampering.”
“These two features of the virus, the mutations in the RBD portion of the spike protein and its distinct backbone, rule out laboratory manipulation as a potential origin for SARS-CoV-2,” wrote Kristian Andersen, associate professor of immunology and microbiology at Scripps Research, and co-leader of the study.
With SARS-CoV-2 virus proliferating around the world, the opportunity arises for further mutations and the emergence of new strains of the virus. This can mean that new virus strains may develop in the future not treatable by possible vaccines that were originally made to treat older strains.
According to Assistant Teaching Professor of Computer Science and Technology Niema Moshiri, COVID-19’s mutation rate is lower than seasonal influenza. The SARS-CoV-2 genome has a limited repair function that edits out most mutations. This has meant the virus has remained relatively uniform.
“What we are finding is that the SARS-CoV-2 virus appears to be mutating more slowly than the seasonal flu which may allow scientists to develop a vaccine,” Moshiri wrote on LiveScience. Despite this, variations do occur, and virologists are constantly looking at the variants to determine if a more virulent strain may be emerging or if the virus is losing its potency.
Scientists are collecting virus sequences and storing them in a globally available database. This is used to determine the rate of mutation and where in the virus genome mutations are occurring. Such mutations can affect the virulence and how effectively the virus can infect human host cells. The existence of different viral strains can be used to trace outbreaks.
Analysis of the SARS-CoV-2 virus from different countries has shown that the virus has undergone several predicted but insignificant mutations already. Scientists led by Peter Forster, along with researchers based in the UK and Germany, traced 160 COVID-19 genomes from China, Europe, and the US. They identified three strains of the virus called A, B and C. Type A is considered to be the original Chinese “ancestral type.” Type B is found in Asia, Europe and the US and has diverged from A with 2 mutations. Type C differs from type B at one site and is mostly confined to Europe and mostly absent from China.
More recently, researchers have alerted that a new strain, D614G, has become dominant in many countries. “The D614G variant first came to our attention in early April, as we had observed a strikingly repetitive pattern. All over the world, even when local epidemics had many cases of the original form circulating, soon after the D614G variant was introduced into a region it became the prevalent form,” wrote theoretical biologist at Los Alamos National Laboratory Bette Korber, in the journal Cell .
“This mutation is present in roughly two third of all global strains,” according to Associate Professor Denis Bauer, transformational bioinformatics team leader at CSIRO’s Australian e-Health Research Centre. The mutation that originated in the virus’ spike protein (not the RBD section) is thought to make it more contagious, but speculation that the virus is more virulent is extremely difficult to prove.
Scientists from the Department of Epidemiology of Microbial Diseases at the Yale School of Public Health led by Nathan D. Grubaugh published a paper in Cell titled “Making Sense of Mutation: What D614G Means for the COVID-19 Pandemic Remains Unclear.” The paper examines whether the strain is more transmissible, infectious, or deadly, but concludes that “these data do not prove that G614 is more infectious or transmissible than viruses containing D614.” They conclude there is no evidence that the virus strain leads “to more severe disease.”
The history of human populations and coronaviruses indicate a possible course for the current pandemic. For instance, the virus OC43 is responsible for the common cold, but a study by researchers from the University of Leuven in Belgium suggest it may have been responsible for a pandemic in 1889 that killed more than 1 million people internationally. They speculate that humans eventually developed immunity against the virus, making future infections more benign.
The course of this pandemic is on par with one of history’s most severe health crisis in modern times. For humanity to develop herd immunity to SARS-CoV-2 would imply untold millions of deaths and incompletely understood chronic health morbidities. Yet, in the 21st century, where scientific knowledge is capable with confronting the threat, capitalism enchains humanity’s ability to respond in kind.
No comments:
Post a Comment